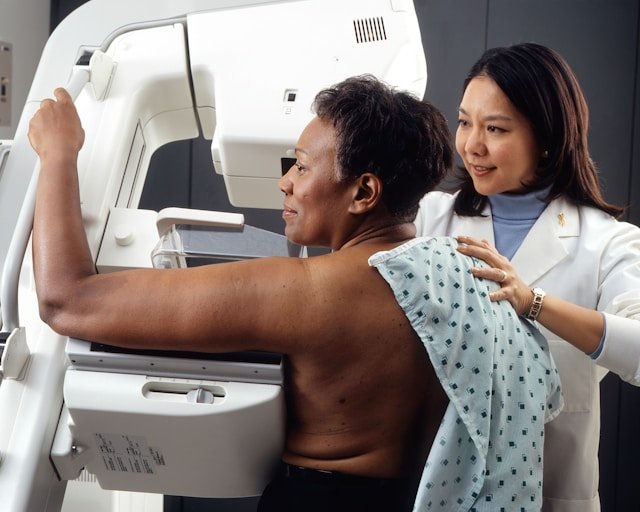
When to Schedule a Mammogram Screening?
Early detection is crucial for effective breast cancer treatment, yet the varied guidelines surrounding mammogram screenings can create uncertainty. This comprehensive guide outlines the latest recommendations to empower you to make well-informed health decisions.
Understanding Mammograms and Their Significance
A mammogram is a specialized X-ray study of the breasts that identifies irregularities or changes in breast tissue before they’re physically noticeable. It stands as the most effective method for the early identification of breast cancer, which can significantly influence the treatment approach—from a straightforward lump removal to a more intensive regimen.
The screening variant of the mammogram captures two X-ray images of each breast to uncover cancer manifestations ahead of symptom emergence. In contrast, diagnostic mammograms are specifically utilized when a doctor or patient observes concerning signs, such as a lump, discomfort, or abnormal discharge from the nipple.
According to the American Cancer Society, the relative five-year survival rate for breast cancer detected at an early stage, before metastasis, is approximately 99%. In contrast, the survival rate declines significantly with later diagnoses. This statistic alone highlights the crucial role that regular mammogram screenings play.
Mammogram Guidelines Based on Age
There isn’t a universally applicable guideline. Here’s how age influences the timing and frequency of screening.
Individuals Under 40
For those under 40, routine mammograms are not typically advised unless there’s a high risk factor present. If you have a familial history of breast cancer, known genetic predispositions such as BRCA1 or BRCA2 mutations, or a past diagnosis of breast cancer, earlier screenings may be necessary. Engaging in a risk assessment discussion with your healthcare provider is essential.
Ages 40-49
This age group presents ambiguous recommendations. Some health organizations advocate for starting annual screenings at 40, while others suggest 45 as the starting age. The best approach involves collaborative decision-making with your doctor, where personal and family histories, lifestyle factors, and overall health are factored into determining an appropriate plan.
Ages 50-74
This demographic typically represents the ideal time for consistent screenings. Most health authorities, including the U.S. Preventive Services Task Force, recommend mammograms every two years for women within this age range. Women at higher risk or who prefer more frequent monitoring may consider annual screenings.
Ages 75 and Above
While screenings can still be advantageous, their necessity often hinges on an individual’s general health and life expectancy. If you are in good health and would consider treatment for any discovered breast cancer, continuing screenings might be warranted. Again, it’s advisable to discuss this with your healthcare provider.
Ultimately, age serves as a general guideline. Individual risk factors should always play a key role in your choices. Lifestyle aspects, such as alcohol use, inactivity, or long-term hormone replacement therapy, can further influence your risk assessment and screening schedule. Talking these points over with your doctor can help create a tailored screening plan that meets your specific needs.
Factors Affecting When to Screen
Age constitutes only one part of the decision-making process. Here are additional considerations that could influence when and how often you should schedule a mammogram.
Family Background
If breast cancer has affected your mother, sister, or grandmother, especially at a younger age, your risk may be significantly elevated. Some specialists suggest initiating screenings 10 years prior to the age your family members were diagnosed.
Genetic Factors
BRCA1 and BRCA2 mutations substantially enhance your lifetime risk for breast cancer. Individuals with these mutations often commence mammograms and MRIs as early as their 30s. If you have concerns about potential genetic predispositions based on family history, consider discussing testing options with your healthcare provider.
Breast Density
High breast density not only elevates cancer risk but also makes tumors more challenging to detect on standard mammograms. If informed of dense breast tissue, a technician might recommend supplementary screenings such as ultrasounds or breast MRIs.
Previous Radiation Exposure
For those who have received chest radiation (commonly for conditions like Hodgkin’s lymphoma) before the age of 30, annual mammograms and breast MRIs should commence eight to 10 years after such treatment.
Ethnic and Racial Considerations
Studies indicate that Black women are more frequently diagnosed with aggressive breast cancer types at younger ages, emphasizing the need for culturally sensitive healthcare and timely access to screenings.
Hormonal Influences
Long-term hormone replacement therapy could increase cancer risk. If you are currently undergoing or have previously utilized hormone therapy, your physician may suggest more regular mammographic assessments.
Every individual presents unique circumstances. Understanding your specific risk factors is the initial step toward establishing an effective and personalized screening strategy. As your risk profile can evolve over time, it’s wise to revisit your screening plan periodically, even if you are already following one.
Indicators for Earlier Screening
Your body may indicate the need for attention before your scheduled screenings. Even if you’re below the recommended age for routine evaluations, the appearance of certain symptoms should prompt you to arrange a mammogram or at least consult with your physician. While these symptoms aren’t always indicators of cancer, they warrant prompt attention:
- Redness, scaling, or flaking of the breast or nipple skin
- A sudden change in nipple shape or inversion
- Persistent pain localized to a specific area
- New lumps or thickening in the breast or underarm
- Swelling or noticeable changes in breast size or shape
- Skin irritation or dimpling
- Discharge from the nipple that is bloody, milky (if not breastfeeding), or clear
While many changes are non-cancerous, an immediate imaging examination can either affirm your concerns or allow for timely intervention if needed. Trust your instincts—do not delay seeking verification by assuming that “it’s probably nothing.”
If you experience any of these symptoms, remain calm but don’t hesitate. Schedule an appointment with your healthcare provider to discuss potential next steps, which might include a diagnostic mammogram, ultrasound, or physical examination. Early action can provide more options and reassurance. In matters of breast health, prompt attention serves as a crucial form of prevention.
Dispelling Common Myths About Mammograms
Misunderstandings should not hinder your access to necessary healthcare. Despite the prevalence of mammograms, numerous myths endure that can deter women from scheduling screenings. Here are some prevalent misconceptions clarified:
- Mammograms are highly painful: Some discomfort due to breast compression is typical, but the process is quick—often just a few seconds per image. Many find that the anxiety leading up to the procedure is worse than the actual experience.
- “I feel fine, so I don’t need one”: The majority of breast cancers do not provide pain or symptomatic indications during their initial stages. This precisely underscores the importance of screenings to identify issues that aren’t visible or detectable.
- They expose you to excessive radiation: Mammograms utilize only a minimal amount of radiation—less than that of a typical chest X-ray—and stay within safety regulations. The advantages of screening outweigh any associated risks.
- Only those with a family history should undergo screening: Most breast cancer cases occur in individuals without any family history. Genetics is merely one of many risk factors.
- “I’m too young or old for a mammogram”: Screening guidelines are determined by risk factors rather than age alone. If you have concerns or symptoms, consult your physician regardless of age.
If uncertain, seek professional advice. It’s preferable to clarify questions than to postpone a potentially life-saving examination due to outdated beliefs. Dispelling these misconceptions fosters a culture of informed patients who prioritize their health.
Preparing for Your Initial Mammogram
You’ve scheduled your appointment—what comes next? Familiarizing yourself with the mammogram process can reduce anxiety and help you feel more prepared. Here’s what you can typically expect.
Pre-Appointment Instructions
Refrain from using deodorants, lotions, or powders on your underarms or breasts as they can interfere with imaging results. Wear a two-piece outfit, as you will need to remove your top. Bring your insurance information along with any previous breast imaging documents, if available.
During the Screening
A technologist (often female) will assist you in positioning each breast onto a flat plate. A second plate will compress the breast briefly to spread out the tissue.
Though it may feel tight or uncomfortable, it should not cause significant pain. You’ll typically undergo two images for each breast—one from top to bottom and the other from side to side.
Post-Exam Follow-Up
You can return to your normal activities right after the exam. Results are generally forwarded to your referring physician within a few hours to a few days, depending on the facility. If any images appear unclear or necessitate further investigation, your provider might request a follow-up diagnostic mammogram or ultrasound.
Many facilities aim to maintain a patient-centered experience, ensuring comfort through a calm environment, compassionate staff, and prompt results. For numerous patients, the anticipation surrounding the exam tends to be more challenging than the procedure itself.
Determining the Ideal Timing for Your Mammograms
Starting with a single mammogram is beneficial, but regularity is crucial. The frequency of your screenings depends on your age, risk profile, medical history, and your healthcare professional’s guidance. Nonetheless, general recommendations provide a useful starting point.
For individuals at average risk:
- Ages 40-49: Recommended every one to two years as per personal risk and individual choice.
- Ages 50-74: Typically advised every two years.
- Ages 75 and older: Screening frequency continues based on personal health and preferences.
For those at higher risk, such as individuals with family histories, genetic mutations, or high breast density:
- Screenings should start earlier, sometimes as early as 30.
- Annual mammograms accompanied by supplementary imaging (like MRIs or ultrasounds) may be necessary.
It’s essential to understand that mammograms do not diagnose cancer; rather, they identify concerns that require additional evaluation. Therefore, adhering to a regular screening schedule is critical, even if you feel healthy. Your physician may also adjust the frequency based on your health status, hormone treatment usage, or past imaging outcomes.
Navigating Mammogram Coverage with Health Insurance
While screenings are vital, will your insurance cover them? In many instances, the answer is yes. Under the Affordable Care Act, most health plans are required to cover screening mammograms for women aged 40 and over on an annual or biennial basis without any out-of-pocket costs. However, specifics can vary based on the insurance provider and plan details. Here are some important points:
- Screening mammograms are typically fully covered.
- Diagnostic mammograms (utilized when there are symptoms or subsequent evaluations are required) might entail co-pays or deductibles.
- Medicare covers mammograms at least once every 12 months for women aged 40 and older.
- If underinsured or uninsured, certain imaging centers offer cash-pay rates or collaborate with nonprofit organizations to assist.
At Envision Imaging, patient-centered care prioritizes your understanding of both your medical and financial options. The center accepts a variety of insurance plans and provides transparent communication about expenses upfront. If you’re unclear on what your plan entails, reach out to your insurance provider, or let your imaging center assist you with the process.
Selecting the Right Imaging Facility
When choosing between different imaging centers, consider the following criteria:
- Accreditation: Ensure the facility holds accreditation from the American College of Radiology or another reputable organization.
- Experienced Personnel: Look for technologists who specialize in breast imaging and board-certified radiologists trained in interpreting results.
- Quick Results: Waiting several days or weeks for results can induce stress.
- Flexible Scheduling: Seek centers offering convenient appointment times, including evenings or weekends.
- Clear Communication: Transparent discussions regarding billing and what to expect during your scan make all the difference.
Take Charge of Your Breast Health
Timing is crucial when it comes to protecting your breast health. Detecting issues early can save lives, and achieving peace of mind begins with taking proactive steps. At Envision Imaging, you’ll receive prompt and accurate results, empathetic care, and an environment designed for your comfort. With flexible scheduling and expert staff, maintaining your health through regular testing has never been more convenient.
Envision Imaging provides top-tier diagnostic services—including mammograms, CT scans, and MRIs—in clean, soothing settings across the southern and western United States. Equipped with advanced technology, quick result times, and compassionate care, it’s never been easier to prioritize your well-being with confidence.
Leading Envision Imaging, Aaron Ramsay draws on over twenty years of expertise in leadership, business strategy, accounting, and financial management as the Chief Executive Officer.





